A Deep Dive into Psoriatic Arthritis and Its Implications

Intro
Psoriatic arthritis is a complex condition characterized by its multifaceted nature. It combines autoimmune elements with joint inflammation and skin lesions. Understanding this intricate interplay requires a focus on several key components: the underlying pathophysiology, the clinical symptoms experienced by patients, diagnostics methods, and the range of therapeutic strategies currently available.
The prevalence of this disease indicates its impact on individual lives and society. It is critical to explore not only the medical aspects but also the socio-economic implications of living with psoriatic arthritis. This exploration will provide insights necessary for both patients and healthcare professionals.
The following sections will delve into crucial highlights of recent research, summarize significant findings, and discuss potential future directions. This comprehensive guide aims to equip readers with a clearer understanding of psoriatic arthritis and the ongoing developments associated with it.
Understanding Psoriatic Arthritis
Understanding psoriatic arthritis is essential in grasping its complexities and implications. This section lays the groundwork for the entire discussion by elucidating what this condition is and why it matters. Psoriatic arthritis intertwines both autoimmune and inflammatory pathways. It not only affects joints but also has skin manifestations, prominently seen in psoriasis.
By comprehending the foundational aspects of psoriatic arthritis, readers can appreciate the interplay between various factors contributing to its manifestation. This knowledge is vital for both patients and healthcare providers. Understanding symptoms, diagnostic methods, and treatment options helps in effective management and improves the quality of life for those affected. Moreover, awareness of this condition can lead to better support systems and resources for patients navigating their health challenges.
Definition and Overview
Psoriatic arthritis is a chronic inflammatory arthritis associated with psoriasis, a skin disease characterized by red, scaly patches. In psoriatic arthritis, inflammation occurs in the joints, leading to pain and stiffness. It can present in various forms, often affecting peripheral joints, the spine, and areas where tendons attach to bones. Patients may experience flare-ups, where symptoms worsen, followed by periods of remission.
Epidemiology
The epidemiology of psoriatic arthritis reveals that it affects approximately 30% of individuals with psoriasis. This rate varies globally, highlighting differences in genetic and environmental factors. Studies indicate that psoriatic arthritis may impact men and women equally, typically developing between the ages of 30 and 50 years.
A thorough understanding of the epidemiological aspects can guide public health strategies and awareness programs aimed at early detection and intervention. Additionally, different populations may exhibit varying disease patterns and severity. This awareness is crucial for tailoring treatments specific to demographic needs.
Pathophysiology of Psoriatic Arthritis
Understanding the pathophysiology of psoriatic arthritis is vital for both clinicians and patients alike. It offers insights into the mechanisms behind this complex disease, guiding treatment strategies and helping to improve patient outcomes. By examining how the immune system, genetic factors, and environmental triggers contribute, one can appreciate the multifaceted nature of the condition. The interplay between these elements is crucial for developing a comprehensive understanding of psoriatic arthritis and informs ongoing research efforts aimed at providing better therapies.
Role of Immune System
The immune system plays a central role in the development and progression of psoriatic arthritis. In patients with this condition, immune responses become dysregulated, leading to inflammation in both the skin and joints. Specifically, T-cells and other immune molecules are activated inappropriately, targeting healthy tissues. This results in chronic inflammation characterized by swelling, pain, and stiffness in joints. Moreover, cytokines such as tumor necrosis factor-alpha (TNF-α) are often elevated, further driving the inflammatory cascade.
"Understanding the immune dysregulation in psoriatic arthritis can lead to targeted therapies, reducing the disease's impact."
New biologic treatments aim to interfere with this immune response, demonstrating the importance of grasping its mechanisms for more effective treatment options. As research progresses, it may unlock even more precise interventions to modulate immune activity in affected individuals.
Genetic Factors
Genetic predisposition is another significant factor influencing the onset and severity of psoriatic arthritis. Studies have identified several genes associated with an increased risk for the condition. Genes such as HLA-B27 and others related to immune responses are frequently implicated. These genetic variants can lead to alterations in immune function and inflammatory pathways, enhancing susceptibility to psoriatic arthritis.
It is important to note that not everyone with a genetic predisposition will develop the disease. Environmental factors often interact with these genetic elements, further complicating the clinical picture. Understanding the genetic underpinnings can provide insight into familial patterns and help identify at-risk individuals for early intervention.
Environmental Triggers
Environmental factors can act as triggers for psoriatic arthritis, especially in genetically predisposed individuals. Several potential triggers have been identified, including:
- Infections: Certain infections, particularly group A streptococcus, have been linked to the onset of psoriatic arthritis.
- Trauma: Physical trauma, such as injuries, can precipitate flares and may even initiate the disease in susceptible individuals.
- Stress: Psychological stress is known to affect immune function and may exacerbate symptoms or trigger disease onset.
- Obesity: Increased body weight has been associated with higher levels of inflammation, which may worsen or trigger psoriatic arthritis.
By comprehensively understanding these environmental triggers, healthcare providers can offer preventive strategies to patients. Strategies may involve educating patients about lifestyle modifications to mitigate risks of flare-ups, as well as addressing psychological health to support overall well-being.
In summary, the pathophysiology of psoriatic arthritis encompasses a complex interplay between the immune system, genetic factors, and environmental triggers. This understanding is not just academic; it has real implications for clinical practices and patient management. By acknowledging these elements, we move closer to personalized and effective treatment approaches.
Clinical Manifestations

Clinical manifestations of psoriatic arthritis play a vital role in understanding this condition. They not only reveal the physical impacts on joints and skin but also offer insight into how psoriatic arthritis affects patients' daily lives. By comprehending these symptoms, healthcare professionals can better tailor treatment plans to individual patient needs. This section will highlight the main symptoms, focusing on articular symptoms, skin involvement, and other related manifestations.
Articular Symptoms
Articular symptoms are prominent indicators of psoriatic arthritis. They commonly include peripheral arthritis, spondylitis, and enthesitis.
Peripheral Arthritis
Peripheral arthritis is often the most noticeable symptom. It involves inflammation of the joints, particularly in the hands and feet. This can lead to pain, swelling, and stiffness, which significantly impacts daily activities. The key characteristic of peripheral arthritis is its asymmetrical nature. This means that one side of the body may be affected more than the other. The presence of peripheral arthritis in this article highlights the importance of early diagnosis. Recognizing these symptoms can lead to prompt treatment, thus avoiding further joint damage.
Advantages of understanding peripheral arthritis include improved patient awareness and management of their condition. However, it can also be a disadvantage because misdiagnosis can occur when symptoms resemble other types of arthritis.
Spondylitis
Spondylitis refers to inflammation in the spinal joints, leading to discomfort and reduced mobility. This form of arthritis usually presents with morning stiffness and can worsen over time. One key feature of spondylitis is its impact on the spine, which can lead to a significant decrease in quality of life. This aspect makes it relevant for this article, as it serves as a reminder of the need for thorough assessments in psoriatic arthritis presentations.
The main disadvantage is that not all healthcare professionals may recognize spondylitis when evaluating psoriatic arthritis. This could prolong the diagnosis and treatment process, ultimately affecting patient outcomes.
Enthesitis
Enthesitis involves inflammation at the sites where tendons and ligaments attach to bone. Common areas for this symptom include the Achilles tendon and the plantar fascia. Unlike other forms of arthritis, enthesitis is particularly painful and can severely limit physical activities. This unique feature is crucial for diagnosis, as early detection can lead to effective intervention strategies. Enthesitis demonstrates the diverse range of symptoms associated with psoriatic arthritis, making it an essential aspect of this discussion.
Advantages of recognizing enthesitis include improved treatment outcomes. On the other hand, the challenge lies in distinguishing enthesitis from other musculoskeletal disorders, which sometimes can complicate diagnosis and management.
Skin Involvement
Psoriatic skin lesions are another prominent manifestation of psoriatic arthritis. The lesions often appear as red patches covered with silvery scales, primarily located on the elbows, knees, and scalp. Skin involvement is a critical indicator of the disease and often precedes or coincides with the onset of joint symptoms. Understanding the skin aspect helps in differential diagnosis and emphasizes the comprehensive nature of psoriatic arthritis, impacting both skin and joints.
Other Symptoms
Other symptoms related to psoriatic arthritis should not be overlooked. They include nail changes, fatigue, and psychological aspects.
Nail Changes
Nail changes might include pitting, discoloration, or separation from the nail bed. This symptom serves as a clear indicator of psoriatic disease when presented with other clinical signs. Understanding nail changes is crucial as they provide valuable clues for proper diagnosis. Some patients may not realize that these changes are linked to an underlying condition. Advantageously, recognizing this can enhance discussions between patients and healthcare providers, leading to better overall care and monitoring.
Fatigue
Fatigue is a common yet overlooked symptom in psoriatic arthritis. Patients often report physical exhaustion alongside joint pain. This symptom is challenging since fatigue can arise from various causes. Recognizing fatigue as a significant aspect of psoriatic arthritis contributes to a better understanding of the holistic impact of the disease. When addressed appropriately, healthcare professionals can help patients improve their energy levels through targeted interventions.
Psychological Aspects
The psychological dimensions of psoriatic arthritis can impact patients’ mental health. Depression and anxiety are more prevalent among those with chronic pain. The understanding of how psychological aspects relate to physical symptoms is vital; addressing mental health can lead to overall well-being. By considering psychological factors, providers can offer a more supportive care model, which ultimately enhances patient outcomes.
Overall, this examination of clinical manifestations emphasizes the multifaceted nature of psoriatic arthritis. From articular symptoms to psychological effects, understanding these aspects is essential for effective management and patient support.
Diagnosis of Psoriatic Arthritis
Diagnosing psoriatic arthritis (PsA) is a crucial component in managing this complex condition. Accurate diagnosis ensures that patients receive appropriate treatment strategies, improving their quality of life. PsA can mimic other forms of arthritis, making it essential for healthcare professionals to conduct a comprehensive evaluation. The diagnosis typically involves a multidisciplinary approach combining clinical assessments, laboratory tests, and advanced imaging techniques.
Clinical Assessment
The first step in diagnosing PsA is a thorough clinical assessment. This involves taking a complete medical history and conducting a physical examination. During this process, the clinician looks for joint swelling, tenderness, and any psoriatic skin lesions. A history of psoriasis in the patient or their family members often provides critical context. Additionally, the clinician evaluates for symptoms often present in PsA, such as fatigue and morning stiffness.
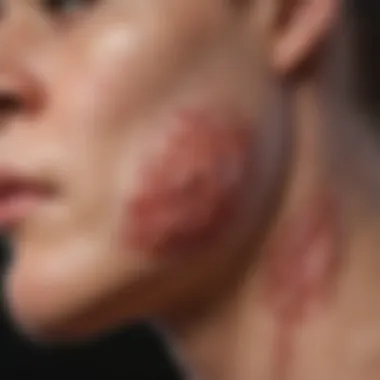

Screening tools like the Psoriasis Area and Severity Index (PASI) can help assess the extent and severity of skin involvement, while other indices focus on the joints affected. Effective clinical assessment is fundamental for differentiating PsA from other arthritic conditions.
Laboratory Tests
Laboratory tests are adjuncts in the diagnostic process of psoriatic arthritis. These tests do not diagnose PsA outright but help in understanding the inflammatory status of the patient. Commonly used tests include:
- Rheumatoid factor (RF): A test for rheumatoid arthritis which is often negative in PsA.
- Antinuclear antibodies (ANA): These may be associated but are typically not specific to PsA.
- Acute phase reactants: Blood tests measuring markers like C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) assess inflammation levels.
Although laboratory tests provide valuable insight, they alone cannot confirm a diagnosis. Their primary value lies in assessing disease activity and tailoring treatment options.
Imaging Techniques
Advanced imaging techniques play a significant role in visualizing changes in joints that may be indicative of psoriatic arthritis. These methods can identify inflammation and structural damage not easily detectable during physical exams. Imaging techniques include:
X-rays
X-rays are often the first imaging modality used in the diagnosis of PsA. They can reveal joint damage and help differentiate between PsA and other types of arthritis. One key characteristic of X-rays is their ability to depict structural changes such as joint erosion or calcification.
X-rays are popular due to their availability and low cost. However, they may miss early signs of disease, and the interpretation depends on the expertise of the radiologist.
Ultrasound
Ultrasound is increasingly utilized in rheumatology due to its ability to visualize soft tissue and joint inflammation. This method can detect synovitis and enthesitis, common features of PsA. A unique advantage of ultrasound is that it offers real-time imaging and can be performed at the bedside.
However, its efficacy greatly relies on the operator’s skill. While it is advantageous for assessing inflammation, it may not fully capture the structural changes seen in advanced stages of the disease.
MRI
Magnetic Resonance Imaging (MRI) provides a comprehensive view of joint structures and is especially useful for observing bone marrow edema, indicative of inflammation. The key characteristic of MRI is its ability to visualize soft tissues in detail. It is beneficial in assessing spondylitis and sacroiliitis, which are important in PsA.
Despite its strengths, MRI is more costly and less accessible than X-rays and ultrasound. Moreover, the interpretation requires specific training, which can limit its regular use in clinical practice.
Treatment Approaches
Treating psoriatic arthritis requires a comprehensive strategy. This multifaceted condition involves various treatment modalities that address both the symptoms and the underlying disease processes. The goal is to enhance patient quality of life while managing inflammation and joint damage.
Pharmacological Treatments
Pharmacological treatments play a significant role in managing psoriatic arthritis. These medications reduce inflammation, control immune responses, and provide relief from pain.
Non-Steroidal Anti-Inflammatory Drugs
Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) are often the first line of treatment. They help reduce inflammation and alleviate pain effectively. The key characteristic of NSAIDs is their ability to inhibit enzymes involved in pain pathways. This makes them a beneficial choice because they can improve function without severe side effects for many individuals. However, long-term use may lead to gastrointestinal issues or cardiovascular concerns, which should be monitored.
Corticosteroids
Corticosteroids can provide rapid relief for inflammation and are useful in acute flare-ups. Their primary attribute is their potent anti-inflammatory effect. Corticosteroids are a popular choice because they can quickly control symptoms. However, the downside is the risk of side effects, especially with long-term use, such as bone loss or weight gain. It is wise to use them cautiously.
Disease-Modifying Antirheumatic Drugs
Disease-Modifying Antirheumatic Drugs (DMARDs) target the underlying disease process and help prevent joint damage. The characteristic feature of DMARDs is their ability to alter the course of the disease. They are a critical option for individuals looking to maintain long-term joint health. The unique aspect of DMARDs is that they often take weeks to months to show effect. Patients might find this delay frustrating, yet they are essential for long-term management.
Biologic Agents

Biologic Agents are advanced treatments designed for patients who do not respond to conventional drugs. Their key characteristic is their tailored action against specific immune pathways involved in psoriatic arthritis. Biologics are beneficial as they can significantly improve quality of life. Each agent targets different parts of the immune system, offering a unique approach. However, they come with risks like increased susceptibility to infections and require monitoring.
Non-Pharmacological Interventions
Non-pharmacological interventions also play a crucial role in managing psoriatic arthritis. These include approaches that can enhance the effectiveness of pharmacological treatments and promote overall well-being.
Physical Therapy
Physical therapy is crucial for maintaining joint function and mobility. It focuses on exercises specifically designed to improve strength and flexibility. The advantage of physical therapy is that it not only addresses physical limitations but also empowers patients by providing skills and strategies for self-management. However, finding a qualified physical therapist who understands psoriatic arthritis is essential for optimal results.
Occupational Therapy
Occupational therapy assists individuals in managing daily activities more effectively. It emphasizes adapting environments and tasks to better suit the individual's capabilities. The significant trait of occupational therapy is its holistic approach, leading to improved daily function and independence. Its unique feature lies in personalized interventions, which can effectively address challenges in personal and work environments.
Diet and Lifestyle Modifications
Diet and lifestyle modifications can have a profound impact on managing psoriatic arthritis symptoms. A well-balanced diet rich in anti-inflammatory foods can help reduce flares. The major characteristic is incorporating healthy nutrition and regular exercise to support immune function and overall health. However, changes require commitment, and results may not be immediate. Education about visible benefits is crucial in encouraging sustained lifestyle changes.
Managing psoriatic arthritis effectively involves a combination of pharmacological and non-pharmacological approaches. Understanding and implementing these strategies empowers patients toward better health and quality of life.
Socio-Economic Implications
Psoriatic arthritis represents not only a clinical challenge but also a significant socio-economic issue. Understanding the socio-economic implications of this condition is crucial for both healthcare providers and patients. This section will delve into the economic burden it places on both individuals and society, as well as its impact on quality of life. These elements are critical for shaping policies and guiding treatment protocols that can alleviate the issues faced by individuals suffering from this disease.
Economic Burden
The economic burden of psoriatic arthritis can be substantial. Patients often deal with high medical costs stemming from various sources. This includes expenses for diagnostics, medications, and specialist consultations. Patients may need rigorous monitoring and frequent visits to healthcare providers, which can lead to additional costs.
- Treatment options such as biologic agents can be very effective but are often expensive. The price of these therapies may strain the financial resources of patients and their families.
- Moreover, indirect costs should not be underestimated. These include lost productivity due to illness, absenteeism from work, and potential early retirement due to chronic pain and functional limitations.
Research suggests that the total annual cost for patients with psoriatic arthritis can be significantly higher than for the general population. The economic impact on healthcare systems also merits attention.
"The average annual cost per patient with psoriatic arthritis can reach thousands of dollars, placing a heavy burden on public health budgets."
Impact on Quality of Life
The impact of psoriatic arthritis on quality of life is profound and multifaceted. Patients experience a range of physical and emotional challenges that can diminish their overall well-being. The chronic pain and disability associated with the disease can limit daily activities, affecting employment and social interactions.
Factors influencing quality of life include:
- Physical limitations: Joint pain and stiffness can interfere with mobility and daily tasks.
- Mental health issues: Individuals might suffer from anxiety and depression due to the chronic nature of the disease and its visible effects, such as skin lesions.
- Social isolation: The visible symptoms can lead to stigmatization and withdrawal from social settings, further complicating emotional health.
The importance of recognizing these quality of life issues cannot be overstated. Addressing them requires a multidimensional approach, including psychosocial support and educational resources for patients and families. When healthcare systems consider both the economic and emotional costs of psoriatic arthritis, they can better allocate resources and foster holistic patient care.
Future Directions in Research
The field of psoriatic arthritis (PsA) is rapidly evolving, and future research offers significant potential to deepen understanding and improve treatment. This exploration focuses on emerging therapies, genetic studies, and longitudinal studies. Each element plays a crucial role in uncovering the complexities of PsA and promoting advancements in patient care.
Emerging Therapies
Research on emerging therapies is pivotal in psoriatic arthritis. New biological agents and small molecules have shown promise in addressing unmet needs. Unlike traditional treatments, these therapies target specific pathways involved in inflammation. For instance, newer biologics like IL-17 and IL-23 inhibitors show efficacy in not only alleviating joint pain but also improving skin conditions associated with PsA. These therapies provide hope for patients not responding to standard treatments. Continuous trials contribute valuable data on safety and effectiveness. The potential for combination therapies also exists, which could enhance response rates and overall effectiveness.
Genetic Studies
Genetic studies are central to understanding the hereditary nature of psoriatic arthritis. Genetic markers can provide insights into disease susceptibility and progression. Research indicates that certain genes associated with the immune system may increase the risk of developing PsA. For example, the HLA-B27 antigen is frequently studied. Exploring genetic predispositions can lead to personalized medicine approaches. Tailoring interventions based on genetic profiles could improve treatment outcomes significantly. Moreover, understanding these genetic factors can help clinicians identify at-risk individuals, enabling earlier and potentially more effective interventions.
Longitudinal Studies
Longitudinal studies are essential for capturing the disease's progression over time. These studies help in understanding the natural history of psoriatic arthritis. They can reveal patterns in symptoms, treatment responses, and the impact of various factors on disease trajectory. By following cohorts of patients, researchers gather data on long-term outcomes, including joint damage and quality of life. Insights from these studies guide clinical practice. They support the establishment of best management strategies and highlight the importance of timely interventions.
"Future research in psoriatic arthritis is not just about treatments; it is about understanding the disease on a fundamental level and improving the lives of those affected."







